

· By Courtney Mayszak, RDN, LDN
Lifting the Period Burden
Periods can be heavy, and not just in terms of flow. Sure, there’s the blood. And then there’s so much more than that.
It’s time to fully acknowledge the toll periods take on the lives of menstruating people. It’s time to recognize that too often, periods are not a minor, invisible inconvenience, despite our best efforts to make them seem that way. Due to the lack of proper education, societal support, and nourishing care for menstrual health, periods have become a public health crisis that can cost us our mental and physical wellbeing, relationships and self-esteem, ability to learn and earn money, and general health and vitality.
We’re tired of suffering silently. So we’re calling it out and giving it a name: the Period Burden.
What’s the Period Burden?
The Period Burden[thuh peer-ee-uhd bur-dn]
noun.
1. The cumulation of the physical, mental, and socio-economic tolls periods can take over the course of a person’s approximate 35-year reproductive life.
Virtually everyone who’s ever menstruated—roughly half the global population—has borne the Period Burden in some way: as lost comfort, ease, happiness, time, opportunity, dignity, income, or all of the above.
Let’s explore how this burden can manifest on different levels. How many can you relate to?
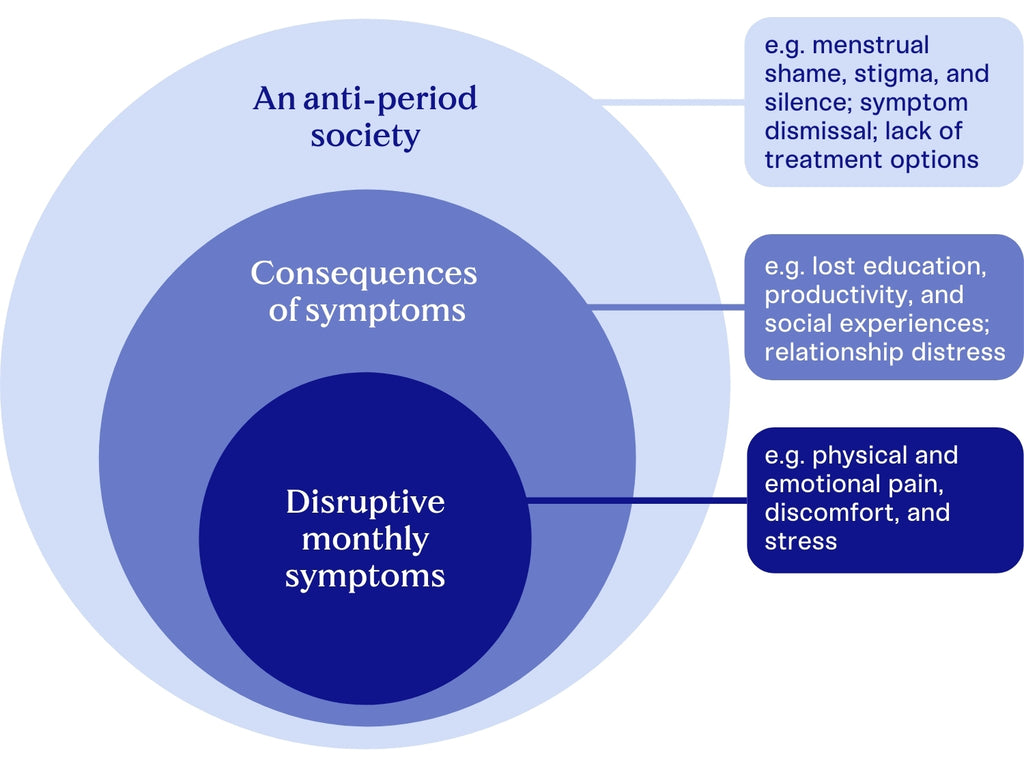
The burden of the symptoms
Over 90% of people with periods endure at least one difficult menstrual symptom each month. At best, it's annoying. At worst, it's straight up disabling. Up to 36% of people with period cramps get severe pain—pain scores of 8-10 on a 10-point scale, with 10 being the worst pain imaginable.
A full mood, brain, and body experience
Few health conditions, gynecological or otherwise, affect as many different parts of the body and mind as Premenstrual Syndrome (PMS). Scientists have identified as many as 150 possible PMS symptoms, but only a subset of them are common. They’re physical (e.g. pain, fatigue, bloating, nausea, constipation, diarrhea), emotional (e.g. mood swings, saddness, irritability), behavioral (e.g. cravings, insomnia), and cognitive (e.g. poor concentration, changes in libido). PMS moderately or severely affects daily activities in up to 35% of people with periods.
Downstream impacts
Period problems can be bigger than your bleeding days. Period pain is associated with reduced quality of life, more psychological distress, and more sleep disruption. People with PMS experience higher rates of social unease, and report that their relationships deteriorate when it strikes.
The burden of missing out
Starting at puberty and lasting well into the peak professional years, people with periods are too often playing academic and professional catchup with their non-menstruating peers.
Stalled workflow
Take pride in your work ethic? Period cramps are the leading cause of missed school and work in women under 30. “But I’ll just power through,” you say, nose to the grindstone. Not so fast: period cramps do seven times more damage through “presenteeism”—a loss of productivity at work from pain and discomfort. 70% of people with PMS and 42% of people with cramps report that their symptoms affect their ability to do their job, which can mean smaller paychecks, more work stress, and a stained professional reputation. All on top of a gender wage gap.
Bleeding the time away
31% of women report spending an average of nearly 10 days in bed each year because of their period. From puberty to menopause, that’s about 350 days—almost a year of life. While there’s certainly no issue with spending a day in bed when that’s your choice, the burden lies in not having a choice, and missing out on things you’d rather be doing like creating, socializing, or moving your body. How would you spend that time if you could reclaim it?
The burden of being silenced
Periods have been shrouded in stigma since the dawn of womankind. Period taboos permeate like cultural osmosis, seeping into our psyche and language, and preventing us from demanding more knowledge, more research, and better care. The silence strips us of our power.
Hiding that you’re hiding it
No matter where you got your sex ed, one of the first things you probably learned about menstruation is that it’s private, even filthy. If your period is invisible, you’re doing it right. So we whisper, speak in euphemisms, and stuff our pads up our sleeves. The shame is stressful, and comes with a psychological toll. What if I leak? What if they know? What if?
Normalizing pain
Period symptoms are extremely common, and when mild to moderate in nature, are part of an otherwise healthy reproductive system. But too often, the word “common” is casually swapped for “normal”, even when describing more severe symptoms. Things get dicey in that interchangeability. Because when we describe a miserable experience as “normal”, we normalize being miserable. Our cultural conversation falls into a trap of backwards psychology, where crippling symptoms are somehow forgivable because they happen on a regular basis. We risk accepting our symptoms as something that’s “supposed to” happen to us, and miss out on proper menstrual health as a result.
The burden of being dismissed
Society’s perceptions of menstrual symptoms have been rooted in gender bias for centuries. In ancient Egypt and Rome, PMS was dismissed as a figment of female craziness, and assigned the term “hysteria”. Hysteria stuck as the medically-recognized term for PMS until the 1930s. Too many people still hear “it’s all in your head” or “you’re just emotional” in response to their menstrual complaints. And the only thing worse than dealing with period problems is having to convince someone—especially your doctor—that you’re not making them up.
Fear of being doubted or denied may help explain why 90% of menstruating people get at least one PMS symptom each month, yet only 10-15% seek medical assistance. When doctors fail to take menstruating peoples’ words at face value, it damages quality of care, health outcomes, and peoples’ relationship with the healthcare system overall.
Left high and dry
We asked our community to share their experiences communicating their period pain to their doctors. Here’s what they told us:
-
“I was told you’re supposed to have period pain and deal with it for sometimes 20 years before someone diagnoses you.”
-
“Early on I was told that periods just hurt. And I should use a heating pad. 🙄”
-
“If they had paid attention… I wouldn’t have suffered so long.”
"Every woman should be the expert of their bodies. When you think your normal pattern is off, it’s off!”
- Dr. Ruth Arumala, OB/GYN, DO, MPH, NCMP
An unsatisfying status quo
Despite how widespread and disruptive period pain is, the generic painkillers used to treat it haven’t advanced since the 1970s. Because drug dosages have historically been based on data collected exclusively in men, women are twice as likely to suffer side effects of medications, including from over-the-counter painkillers: the status quo option people relied on to make period cramps endurable. Until now.
Lifting the Period Burden
Between the neglected symptoms, loss of opportunity, and paralyzing stigma, the Period Burden drains millions of menstruating people of their inherent, uninhibited vitality.
We won’t stand for it any longer.
De Lune is here to lift the Period Burden. We serve the 50 million Americans who suffer from disruptive monthly period symptoms and want a more empowering, nontoxic approach.
At De Lune, menstrual wellness is supported and celebrated. Natural, research-backed relief is the norm, period-positive conversations flourish, and your symptoms never hold you back. Your period arrives each month with a sense of mastery—a life-affirming reminder that you’re strong, powerful, and in sync with nature.
The menstrual revolution is here, and it’s long overdue. Welcome to the New Age of Period Health.

